Personal Protective Equipment (PPE) is fundamental to lessen the risk of exposure to the virus for all who are attending to the health and well-being of COVID-19 patients in various care settings. The speedily diminishing supply of PPEs available for the healthcare workforce, combined with challenges with the supply chain, has justifiably caused widespread distress and could considerably hinder our ability to ensure the safety of those who have committed to the safety of others.
Healthcare organizations have not encountered a supply chain disruption of this magnitude before. That’s why they have partnered with innovators and businesses like ours to attempt to ensure an adequate supply of PPEs during the duration of the pandemic, but until these efforts ramp up sufficiently to meet the needs, current supplies continue to diminish forcing many health care organizations to make difficult decisions about how to conserve existing supplies.
That’s why we want to share some common tactics that many systems are currently using in the hopes that they will be helpful to your efforts. The approaches below are taken from interviews, writings, and exchanges amongst healthcare organizations in the US.
PPE conservation strategies are divided into three parts: Restrict Reduce and Reuse.
Restrict
Restrict or minimize the number of entrances to healthcare settings and screen all visitors for symptoms. Create standardized workflows for screening and communication with visitors.
Consider specific units or areas for Persons Under Investigation (PUI) and COVID-19 individuals with dedicated care teams.
Bundle as many tasks together as possible, if two people are required, ensure they can group and complete all necessary tasks at one entry.
If feasible, have care teams do some of the routine cleanings after patient care so that environmental services only do terminal cleans.
Keep PPEs in centralized locations with individuals from quality or infection control departments responsible for distribution.
Reduce
Eliminate elective surgeries and procedures and minimize unnecessary face to face encounters.
Reduce the potential for viral exposure through physical controls to separate COVID-19 patients.
Isolate PUIs with proper ventilation systems and put surgical masks on PUI and COVID-19 only when they are not isolated.
Develop an inventory system to identify high use areas and ensure appropriate use. Accurate inventory will allow mobilization to high-risk areas when inventory is low and mitigate rationing.
Re-Use
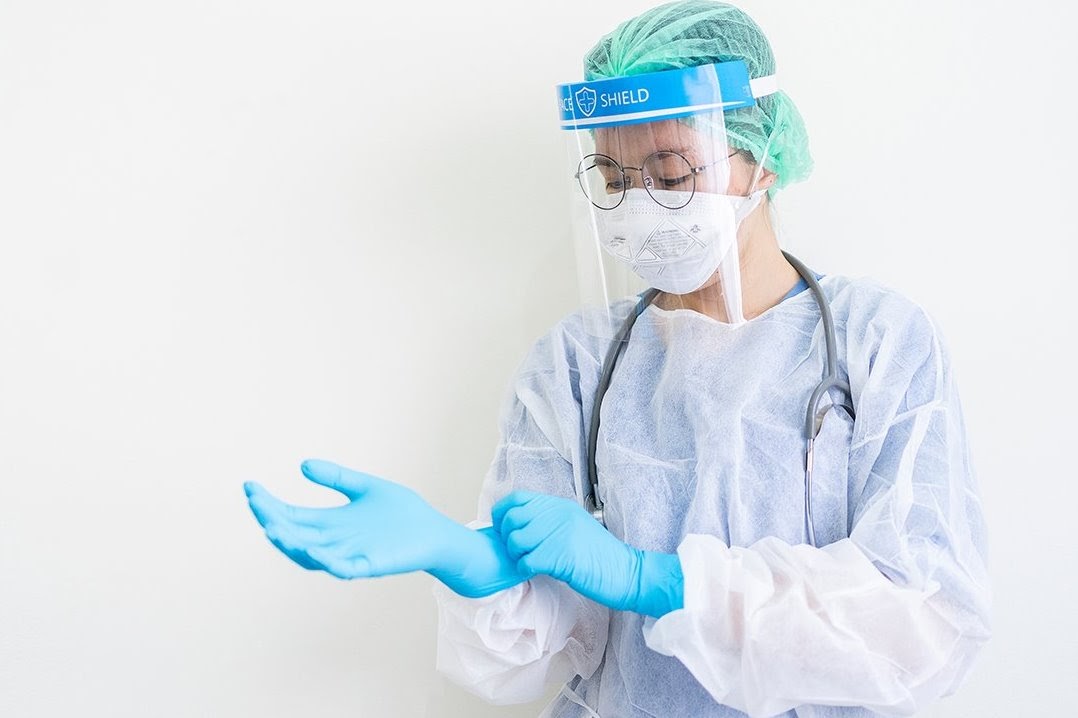
Extend the wear of N95s and facemasks from patient to patient with the clinician changing gown and gloves between patients.
Re-use their N95 up to 5 times if it has been covered by a facemask and is clean and not wet or soiled. Masks are stored in a paper bag with 5 checkbox notations on the outside of the bag.
For all such approaches, consider developing a chart for staff with clear guidelines regarding what items should be used by whom and under what circumstances in addition to when they can be re-used and/or parameters for extended use.
Conclusions
The provision of PPE is an essential aspect of our healthcare system throughout the pandemic. Having appropriate supply, proper use, and a clear PPE strategy during the COVID-19 pandemic is the only way to keep patients and healthcare workers safe.
At We Shield, we work hard to create a safe and clean environment for our front line workers and patients fighting COVID-19 by sourcing and distributing top-quality personal protective equipment and safety supplies at the best pricing on the market.
